Stemming The Tide Of Hypertension In Women: Optimal Age For Obstetric Debut
Abstract
Objective
Women have continued to bear a heavy burden of cardiovascular disease morbidity and mortality with hypertension as the flagship. This is partly because as the modifiable cardiovascular disease risk factors are falling in rate, gender specific risk factors have persisted. One of them is age at first pregnancy and delivery.
Methods
In order to contribute to this discourse, we secondarily analysed data generated in a previous field study on risk factors for cardiovascular diseases in free living adults in Plateau State, Nigeria. The women were divided into four groups and we looked at blood pressure at the time of study from the perspective of age at first pregnancy.
Reults
It was found that those who had their first pregnancy in the late teenage years had the lowest mean arterial blood pressure many years down the line; better than those who started child bearing earlier and those who started later. There was also significant within and between group differences in the blood pressures (p = 0.000).
Conclusion
To stem the tide of female hypertension later in life, child bearing should not start in the early teenage years nor be unnecessarily delayed. Sociocultural conditions that promote early teenage marriage and pregnancy should be discouraged.
Author Contributions
Academic Editor: Sanjeev Chaudhary, Associate Professor, Government Medical College, Nagpur, Maharashtra, India
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2023 Basil N Okeahialam
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Cardiovascular diseases (CVD) constitute a leading cause of morbidity and mortality globally..1 The consequent burden in economic terms is huge; and any steps that can mitigate it is desirable. The risk factor with the most robust evidence for causation of CVDs is hypertension. 2 In pregnancy, associated hypertension is one of the health encumbrances with adverse outcome in both mother and child. 3 Additionally, any hypertension in pregnancy raises the risk of CVD in later life of the women. 4 As a result, any steps taken to prevent hypertension in pregnancy will go a long way in ensuring overall maternal and female gender health. Child bearing early in adolescence is associated with hypertension both during the pregnancy 5 and later in life. 6 Young age at first delivery has been linked with incident CVD. 7
As posited by Datta et al 6 the effects of early child bearing in resource constrained settings where child marriage is acceptable is not well characterized. This study therefore attempts to determine at what age first pregnancy will be desirable in order to stem the tide of hypertension in women with a view to mitigating its short and long term sequelae in such an environment. That black women are known to bear the burden of cardiovascular morbi-mortality largely because of ethnicity and socio-cultural practices. 8 makes such study very relevant. It is data from such studies that will drive initiation of sustainable solutions to address identified socio-cultural determinants of health
Materials and methods
We secondarily analysed data generated in our 2008 field study of Cardiovascular epidemiological transition in Mangu local government area of Plateau State Nigeria, details of which had been published earlier. 9 The focus was to see how blood pressure in adult females related to age at first pregnancy. The main study was approved by the Research and Ethics Committee of Jos University Teaching Hospital and all subjects voluntarily responded to the invitation for cardiovascular diseases risk assessment consenting to be included in the study. Briefly on each of the days of field survey, adult residents of the community who responded to our invitation through their community leaders were registered in order of arrival. After registration, biodata and relevant histories were requested and documented. Blood pressure was estimated by standard anthropometry utilizing the ACCOSON brand mercury sphygmomanometer and appropriate sized cuff by field staff of the registrar rank in the Medical Residency Training Programme. This was after subjects had rested, sitting for 3 to 5 minutes and all necessary precautions taken. Three readings were taken at about 2 minutes interval and the average of the last 2 used for analysis.
To determine age at first pregnancy, we took the age by the last birthday at the point of survey in 2008 from which we subtracted the product of 2 and number of pregnancies. This was predicated on the assumption that on the average, pregnancy occurred in 2 yearly cycles in African women. 10 Subjects were then grouped into four: < 16 years (group 1), 16 – 19 years (group 2), 20 – 24 years (group 3), > 24 years (group 4)
Statistics
Relevant data were subjected to analysis in the Research Support Unit of University of Jos Computer Centre with the SPSS Version 17 software. Continuous variables were expressed as mean + SD. Analysis of Variance (ANOVA) tests were used to assess association between groups and within groups. Finally mean plots were generated for means of blood pressure (Systolic and Diastolic) and age groups at first delivery.
Results
A total of 433 women had complete data to determine age at first delivery They constitute the analyzable population in this case. They were grouped by ages into the following: group 1 (< 16 years), group 2 (16 – 19 years), group 3 (20 – 24 years) and group 4 (> 24 years). The number of subjects in the groups based on age at first pregnancy rose with increasing age. However, adult blood pressure did not follow this trend but was lowest in the 16 – 19 years bracket of group 2. See Table 1. Table 2.
Table 1. Mean Blood pressure of adult women studied based on age at first delivery| Age Group | Age Bracket | Number | SBP | DBP | |||
| 1 | < 16 years | 39 | 117.0 (3.24) | 74.41 (1.82) | |||
| 2 | 16 – 19 years | 91 | 112.14 (1.55) | 72.11 (0.96) | |||
| 3 | 20 – 24 years | 126 | 118.83 (1.59) | 76.15 (0.94) | |||
| 4 | > 24 years | 177 | 129.31 (2.17) | 81.56 (0.98) | |||
| TOTAL | 433 | 121.55 (1.14) | 77.36 (0.58) | ||||
Mean plot graphs Figure 1 (for systolic blood pressure) and Figure 2 (for diastolic blood pressure) capture these graphically
Figure 1.Mean Diastolic Blood Pressure across age group at first delivery
Figure 2.Mean Diastolic Blood Pressure across age group at first delivery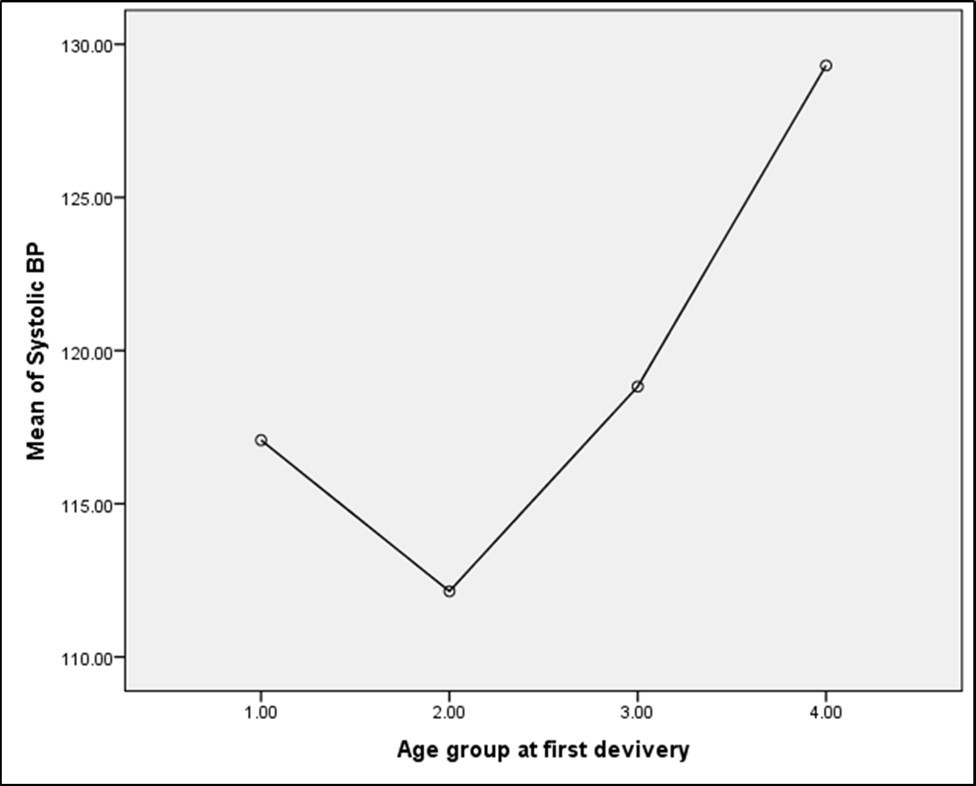
| Sum of squares | df | Mean Square | F | Sig | ||
| Between Groups | 20413.68 | 3 | 6804.561 | 13.162 | 0 | |
| Within Groups | 221791.6 | 429 | 516.997 | |||
| Total | 242205.3 | 432 | ||||
| Between Groups | 6153.13 | 3 | 2051.043 | 15.63 | 0 | |
| Within Groups | 56296.1 | 429 | 131.226 | |||
| Total | 62449.23 | 432 | ||||
Discussion
The results of this study show clearly that in free living adult Nigerian women, the blood pressure in adult life has a relationship with age at first pregnancy. Those women whose first pregnancy fell into the 16 to 19 late teenage bracket, that is group 2 of our study subjects had the lowest mean blood pressure as adults. Mean blood pressure in the early teen age bracket (< 16 years) was higher. First pregnancy after the late teen age bracket was associated with a rise in mean blood pressure in adulthood. This has implication for decision of timing of first pregnancy if burden of blood pressure in adult females is to be mitigated. A few studies were encountered in literature all converging on the fact that the lowest age at first pregnancy had the highest mean blood pressure later in adult life.6, 11, 12, 13
The reasons why this would be so can be fathomed. Pregnancies early in life, just after attaining secondary sexual characteristics is stressful. These are children literally adjusting psychologically to adulthood who are given off in marriage either because of poverty in family or sociocultural beliefs; or who may actually have been taken advantage of. Marriage in such circumstances lead to stress and depression , with the inherent intimate partner violence because of wide age gap with spouses in most cases. 14 Stress and depression are known to initiate hypertension in those with the predisposition. 15 They are also highly prone to obstetric complications like pre-term delivery, low birth weight and eclampsia 16 which have been known to result in higher chances of hypertension after such index pregnancy. 17 We had shown in a previous study on obstetric predictors of hypertension in the post puerperal period (though not only in early life pregnancies) that hypertension in the index or previous pregnancies, premature delivery are red flags for hypertension later in the life of the women. 18 These factors that complicate early life pregnancy have been identified as drivers of CVD development later in life 19, 20 and should warrant ongoing CVD assessment to reduce the incidence.
By the age categorization used in our study, the number of women in the > 24 year bracket for first pregnancy was greater than all the others. Infact there was a gradual rise in number from group 1 to group 4 (Table 1). Interestingly the mean blood pressure, but for the dip in group 2, rose as the age at first pregnancy increased, in contrast with the experience of some workers (Lind, Hennessy and Chin, 2015) where it was highest for the early teenage pregnancy group and reduced with increasing age at first pregnancy. The difference in age categorisations used in the different studies may explain this difference. It is also possible that factors like socioeconomic classification, overweight/obesity, hormonal contraceptive use and educational status differences may account for this. With educational pursuits becoming commonplace, it is proving difficult to have women marry before their early twenties. It must be stated that there is no “best” time to start child-bearing. It is a function of time, tide and clime. The choice is not so much of a voluntary act. The individual may have to pander to career development, financial stability and attainment of personal goals 21 Whereas there is a consensus that starting very early soon after puberty in the early teens is fraught with health and psychological risks, starting very late equally has its own problems. There is the risk of eclampsia, uterine rupture and dysglycaemia 22 as well as slowing societal regeneration. 20
Strenghts and weaknesses
Our study is limited by the following issues. The age at first pregnancy was derived and may not have been very precise. It is a report from a single location which restricts its external validity. Its strength derives from it being a study of free living adult females in populations that are largely understudied, hence presenting a different perspective on the subject.
Conclusion
Early obstetric debut is fraught with medical and psychological complications and should be discouraged. The individuals that start child bearing soon after puberty in early teenages below 16 years apart from the risks they face stand to increase the burden of hypertension in females later in life. Since the burden is also high with late debut, women should strike a balance between career and economic stability with a good time to start child bearing.
Acknowledgement
The expertise of Mr. Toro of the Research Support Unit at the University of Jos, Computer Centre is greatly appreciated.
Declaration Of interest
The original work which data is being secondarily analysed benefited from a research grant (RGC/2008/01) by the Senate Central Research Grant Committee of the University Of Jos, Jos Nigeria
References
- 1.Amini M, Zayeri F, Salehi M. (2021) Trend analysis of cardiovascular disease mortality, incidence and mortality to incidence ratio: results from global burden of disease study. , BMC Public Health 21, 401.
- 2.Fuchs F D, Whelton P K. (2020) High blood pressure and cardiovascular disease. , Hypertens.; 75, 285-292.
- 3.Muti M, Tshimanga M, Notion G T, Bangure D, Chonzi P. (2015) Prevalence of pregnancy induced hypertension and pregnancy outcomes among women seeking maternity services in Harare Zimbabwe. , BMC Cardiovasc Disord 15, 111.
- 4.Alsnes Vatten LJ, Fraser A, Bjorngaard J H, Rich-Edwards J, Romundstad P R. (2017) Hypertension in pregnancy and offspring cardiovascular disease risk in young adulthood. Prospective and siblings studies in the HUNT Study (Nord-Trondeleg Health Study in Norway. Hypertens 69, 591-598.
- 5.Malamitsi-Puchner A, Boutsikou T. (2006) Adolescent pregnancy and perinatal outcome. , Paediatr. Endocrinol. Rev 3, 16641854.
- 6.Datta B K, Hussain M J, Kostova D. (2021) Hypertension in women: the role of adolescent child bearing. , BMC Public Health 21, 1481.
- 7.LeBlanc E S. (2016) Reproductive risk factors and coronary heart disease in the Women’s Health Initiative observational study. , Circ.; 133, 2149-2158.
- 8.Ogunniyi M O, Mahmoud Z, Commodore-Mensah Y, Fleg J L, Fatade Y A et al. (2022) disparities in Cardiovascular disease for Black women: JACC Review Topic of the week. , JACC 80(18), 1762-1771.
- 9.Okeahialam B N, Ogbonna C, Otokwula A E, Joseph D E, Chuhwak E K et al. (2012) Cardiovascular epidemiological transition in a rural habitat of Nigeria. The case of Mangu local government. 31-1.
- 10.Alani M, Mbalinda S N, Muhindo R. (2020) Birth intervals and associated factors among women attending young child clinic in Yumbe hospital Uganda. Article ID: , Int. J. Rep. Med 1326596.
- 11.Park S. (2017) Age at first child birth and hypertension in post menopausal women. Hypertens. 69, 821-828.
- 12.Lind J M, Hennessy A, Chin C L. (2015) Association between a woman’s age at first birth and high blood pressure. , Medicine 94(16), 697.
- 13.Tabeu P M, Foumane P, Mbu R, Fisso G, Biyaji P T et al.(2011).Risk factors for hypertensive diseases in pregnancy: A report from Maroua Regional Hospital. , Cameroon. J. Reprod. Infertil 12(3), 227-234.
- 14.Ahmed S, Khan S, Alia M, Noushad S. (2013) impact evaluation of early marriages. , Int. J. Endorsing Health Sci Res 1(2), 84-86.
- 15.Rubio-Guerra A F, Rodriguez-Lopez L, Vargas-Ayala G, Huerta-Ramirez S, Serra D C et al. (2013) Depression increased the risk for uncontrolled hypertension. , Exp. Clin. Cardiol.18(1): 10 – 12.
- 16.Todhunter L, Hogan-Roy M, Pressman E K. (2022) . , Complications of pregnancy in Adolescents. Semin. Reprod. Med 40-1.
- 17.Ahmad A, Oparil S. (2017) Hypertension in women. Recent advances and lingering questions. Hypertens. 70: 19 – 26
- 18.Agbo H A, Okeahialam B N, Daru P H. (2016) Obstetric predictors of hypertension: a cross-sectional study of women attending the post-natal clinic of Jos University Teaching Hospital. Niger Med. , J 57(6), 320-323.
- 19.Minissian M B, Kilpatrick S, Eastwood J A, Robbins W A, Accortt E E et al. (2018) Association of preterm delivery and future maternal cardiovascular disease. Circ. 137-865.
- 20.Leon M J, McCarthy F P, Direk K, Gonzalez-Izquiredo A, Prieto-Merino D et al. (2019) Preclampsia and cardiovascular disease in a large UK pregnancy cohort of linked electronic health records: A CALIBER Study. Circ.140: 1050 – 1060.
